
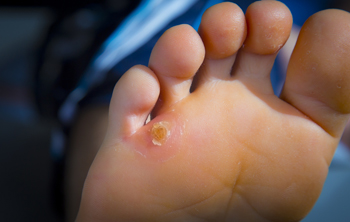
 Foot corns occur when the foot is exposed to the friction of skin rubbing against the bone, shoe, or ground. They are similar to calluses and create a thick layer of hard skin on the sole of the foot or in between toes. Corns more specifically occur on top of bones and joints. They have a central core, which has the possibility of resulting in pain if it presses on a nerve. There are many home remedies for treating foot corns. Carefully rubbing the area with a pumice stone or chiropody sponge after soaking your feet and regularly moisturizing can help remove the hard-thickened skin over time. Be wary of over-the-counter corn plasters if you have sensitive skin, because they contain high levels of salicylic acid. If you have corns on your feet, it is suggested that you consult with a podiatrist to find out which treatment option is best for you.
Foot corns occur when the foot is exposed to the friction of skin rubbing against the bone, shoe, or ground. They are similar to calluses and create a thick layer of hard skin on the sole of the foot or in between toes. Corns more specifically occur on top of bones and joints. They have a central core, which has the possibility of resulting in pain if it presses on a nerve. There are many home remedies for treating foot corns. Carefully rubbing the area with a pumice stone or chiropody sponge after soaking your feet and regularly moisturizing can help remove the hard-thickened skin over time. Be wary of over-the-counter corn plasters if you have sensitive skin, because they contain high levels of salicylic acid. If you have corns on your feet, it is suggested that you consult with a podiatrist to find out which treatment option is best for you.
If you have any concerns regarding your feet and ankles, contact Dr. Alan J. Spector of Shore Podiatry. Our doctor will treat your foot and ankle needs.
Corns: What Are They? and How Do You Get Rid of Them?
Corns can be described as areas of the skin that have thickened to the point of becoming painful or irritating. They are often layers and layers of the skin that have become dry and rough, and are normally smaller than calluses.
Ways to Prevent Corns
There are many ways to get rid of painful corns such as wearing:
Treating Corns
Treatment of corns involves removing the dead skin that has built up in the specific area of the foot. Consult with Our doctor to determine the best treatment option for your case of corns.
If you have any questions please feel free to contact our office located in Point Pleasant, NJ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Corns and Calluses are both hardened layers of thickened skin that develop because of friction. Both ailments are typically found on the feet and may be unsightly. Although they have similarities, corns and calluses are different from each other.
Some causes of corns and calluses may be wearing ill-fitting shoes and not wearing socks. If you wear tight shoes, your feet will constantly be forced to rub against the shoes, causing friction. If you fail to wear socks, you are also causing your feet to endure excess friction.
There are some signs that may help you determine whether you have one of these two conditions. The first symptom is a thick, rough area of skin. Another common symptom is a hardened, raised bump on the foot. You may also experience tenderness or pain under the skin in addition to flaky, dry, or waxy skin.
There are also risk factors that may make someone more prone to developing corns and calluses. If you are already dealing with bunions or hammertoe, you may be more vulnerable to having corns and calluses as well. Other risk factors are foot deformities such as bone spurs, which can cause constant rubbing inside the shoe.
Corns tend to be smaller than calluses and they usually have a hard center surrounded by inflamed skin. They also tend to develop on the parts of the body that don’t bear as much weight such as the tops and sides of toes. Corns may also be painful for those who have them. On the other hand, calluses are rarely painful. These tend to develop on the bottom of the feet and may vary in size and shape.
Fortunately, most people only need treatment for corns and calluses if they are experiencing discomfort. At home treatments for corns and calluses should be avoided, because they will likely lead to infection. If you have either of these ailments it is advised that you consult with your podiatrist to determine the best treatment option for you.
In 2014, the American Podiatric Medical Association surveyed 1,000 American adults and found that half of all respondents lived with foot pain. Fortunately, there are ways to avoid foot problems such as following a daily footcare routine and wearing proper footwear at work.
If you have a job that requires you to be on your feet, it is best that you do not wear flat sole shoes. Your heel should be slightly elevated (less than 2 inches, but at least ¼-inch) if you are going to be standing for a prolonged period. You should also make sure that the shoes you wear are not too small. Tight shoes may cut off circulation to your feet, which will result in pain and blisters. It is always best to purchase fitted shoes later in the day, because the feet tend to swell as the day progresses. It may also be helpful to buy shoes a half size larger if you plan on wearing custom orthotics or arch supports.
Your muscles may become stiff when you are constantly standing up. It is important to take breaks every hour to stretch and relax. One tip is to perform calf raises, because this exercise will help improve your circulation. To perform this stretch, you first need to stand on the edge of a step with your abdominal muscles pulled inward. You then need to grip the step with the balls of your feet with your heels hanging over the edge. Next, try to raise your heels above the step by a few inches while standing on your tiptoes; hold this pose for a second. You should then lower your heels back even to the platform. These calf raises should be done ten times for full effectiveness.
You should also take care of your feet while you are at home. One of the best ways to prepare your feet for a long day of work is to soak them in ice water. Doing so for 20 minutes will help fight the swelling and inflammation that results from being on your feet at work.
Nevertheless, if you are experiencing pain in your feet, you should seek help from your podiatrist. Your doctor will help treat any ailments you may have in addition to helping you prevent any other ailments from developing in the future.
 Many people are involved in jobs where standing is mandatory for most of the day. There may be methods that can alleviate any foot pain, which may be present while working, including using shoe inserts, standing on stress mats instead of hard flooring, or wearing compression stockings. Additionally, it may be beneficial to change positions frequently during the day, which may include sitting for short periods at a time and performing gentle stretches. Wearing shoes that are comfortable and fit well may aid in diminishing aches and pains the feet may endure. Research has shown it may be best to try shoes on after the work day is completed, and this may allow for any swelling that may be present. Properly taking care of your feet while completing the work day may help to prevent painful foot conditions, including plantar fasciitis and Achilles tendinitis. If you would like additional information about the importance of protecting your feet while working, please consult with a podiatrist.
Many people are involved in jobs where standing is mandatory for most of the day. There may be methods that can alleviate any foot pain, which may be present while working, including using shoe inserts, standing on stress mats instead of hard flooring, or wearing compression stockings. Additionally, it may be beneficial to change positions frequently during the day, which may include sitting for short periods at a time and performing gentle stretches. Wearing shoes that are comfortable and fit well may aid in diminishing aches and pains the feet may endure. Research has shown it may be best to try shoes on after the work day is completed, and this may allow for any swelling that may be present. Properly taking care of your feet while completing the work day may help to prevent painful foot conditions, including plantar fasciitis and Achilles tendinitis. If you would like additional information about the importance of protecting your feet while working, please consult with a podiatrist.
While working on the feet, it is important to take the proper care of them. For more information about working on your feet, contact Dr. Alan J. Spector from Shore Podiatry. Our doctor will treat your foot and ankle needs.
Working on Your Feet
Standing on your feet for long periods of time can cause stress and pain in your feet. Your whole body may experience change in terms of posture, back pain, bunions, callouses and or plantar warts. There are ways to avoid these conditions with proper foot care, smart choices and correct posture.
Positive Changes
Negative heeled shoe – Choosing this shoe type places the heel slightly lower than the ball of the foot. These are great for overall foot health. Find shoes that fit you correctly.
Go barefoot – Our feet were not designed to be enclosed for all hours of the day. Try to periodically expose your feet to air.
Eliminate Pain
Foot Exercises – Performing simple exercises, incorporating yoga and doing stretches are beneficial. This will allow increased blood flow to the area and muscles of the foot.
Achilles tendon – Stretching the foot out flat on the floor will relax the calf muscles and tendon. These exercises can be performed almost anywhere. Make sure you add these exercises to your daily regimen.
With a little bit of this information and knowing more about foot health, you will notice changes. Foot stretches and proper footwear will help with pain and prevent further issues.
If you have any questions please feel free to contact our office located in Point Pleasant, NJ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Elderly Americans are very susceptible to falls as they get older. Everyone experiences decreases in flexibility, balance, strength, and the senses as they age. This correlates to some eye-opening statistics. 1 in 4 Americans aged 65 and older fall each year. An elderly American is being treated for a fall in an emergency room every 11 seconds, and every 19 minutes, an older person dies from falling. In light of these striking statistics, one can see the importance of taking steps to prevent falls.
Finding an exercise program for the elderly is an excellent way to reduce the likelihood of falls. Look for an exercise program that improves strength and balance. Elderly people who live a more sedentary lifestyle, with little physical activity, are at an increased risk of falling. Wearing well-fitted footwear that provides good foot support and cushion will help prevent falls from poorly fitted shoes. Talking to a podiatrist about your susceptibility to falls and about inspecting your prescriptions will help to avoid any medication that could make falls more likely. Due to a decline in the senses among the elderly, having your eyes and hearing checked is recommended.
Around half of all falls occur in the household. Removing tripping hazards in the home and making it more accommodating to older persons can significantly reduce falls. Some notable household changes include increasing lighting around the house, installing grab bars in the shower and bathroom, and making sure the floor is clear of clutter. Other smart options include installing a shower chair, using rubber-bottomed rugs, and placing railings on both sides of stairwells.
Finally, discuss with a doctor and your family about your fear of falling. This will help to increase awareness among the population on the need for fall prevention. A lack of awareness on the matter, and a downplaying of importance are what increase the risks of falling. Following these tips can help to reduce the risk for yourself and your loved ones.
 Research has shown the unnatural act of falling may be common among senior citizens. According to a portion of an AARP bulletin, deaths from falling is among the highest in the cold states of Wisconsin and Minnesota. In places where there may be an accumulation of snow, it may be beneficial to wear shoes that have traction or cleats, and this may aid in preventing any falls that may occur. If you must walk outside for extended periods of time, it may be helpful to look at your pathway a few steps in advance, and this may prevent any slipping on black ice. In addition to properly preparing your trek outside, it is important to check the condition of your home and remove items that may cause tripping. These may include repairing or replacing any loose carpeting and moving any extension cords that may be a falling hazard. If you have endured a fall and have injured your ankles or feet, it is suggested to speak with a podiatrist so proper treatment can begin.
Research has shown the unnatural act of falling may be common among senior citizens. According to a portion of an AARP bulletin, deaths from falling is among the highest in the cold states of Wisconsin and Minnesota. In places where there may be an accumulation of snow, it may be beneficial to wear shoes that have traction or cleats, and this may aid in preventing any falls that may occur. If you must walk outside for extended periods of time, it may be helpful to look at your pathway a few steps in advance, and this may prevent any slipping on black ice. In addition to properly preparing your trek outside, it is important to check the condition of your home and remove items that may cause tripping. These may include repairing or replacing any loose carpeting and moving any extension cords that may be a falling hazard. If you have endured a fall and have injured your ankles or feet, it is suggested to speak with a podiatrist so proper treatment can begin.
Preventing falls among the elderly is very important. If you are older and have fallen or fear that you are prone to falling, consult with Dr. Alan J. Spector from Shore Podiatry. Our doctor will assess your condition and provide you with quality advice and care.
Every 11 seconds, an elderly American is being treated in an emergency room for a fall related injury. Falls are the leading cause of head and hip injuries for those 65 and older. Due to decreases in strength, balance, senses, and lack of awareness, elderly persons are very susceptible to falling. Thankfully, there are a number of things older persons can do to prevent falls.
How to Prevent Falls
Some effective methods that older persons can do to prevent falls include:
Falling can be a traumatic and embarrassing experience for elderly persons; this can make them less willing to leave the house, and less willing to talk to someone about their fears of falling. Doing such things, however, will increase the likelihood of tripping or losing one’s balance. Knowing the causes of falling and how to prevent them is the best way to mitigate the risk of serious injury.
If you have any questions, please feel free to contact our office located in Point Pleasant, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Rheumatoid Arthritis is a chronic progressive disease that attacks several joints throughout the body. It is an autoimmune disease in which the body’s immune system mistakenly attacks the joints. As a result, the tissue inside the joints, called synovium, starts to thicken and causes pain around the joints. The synovium is responsible for creating a fluid that lubricates the joints to help them move. Approximately 1.5 million people in the United States have Rheumatoid Arthritis. Women are almost three times as likely to have RA compared to men, and it’s disease usually begins between the ages of 30 and 60. People who have a genetic history of RA are more likely to develop the disease.
Symptoms of RA may include the following sensations in the joints: pain, tenderness, swelling, redness, warmth, stiffness, and loss of range. Swollen joints are a very common symptom for those with the disease. At times, it may be minimal, but it may also be very apparent. Another typical symptom is joint stiffness. Doctors will often use the direction of morning stiffness to measure the severity of a patient’s joint inflammation. Other RA symptoms include limping, anemia, fever, and fatigue.
To diagnose RA, your podiatrist will typically request x-rays to see how much damage there is in the joints. Blood tests may also be performed to show if there are any signs of anemia, or antibodies such as the rheumatoid factor. If you have previously been diagnosed with RA, you should know the disease may spread to your feet and ankles.
There are many non-surgical options that can be used to treat this ailment. Some of these options include physical therapy, foot massages, orthotics, bracing, supportive shoes, and steroid injections. Physical therapy is useful because it will help stretch and strengthen the joints in both the foot and ankle to improve joint function. Massages can help improve blood circulation which will be good for the feet. Choosing proper footwear will allow you to walk with comfortability if you are a sufferer from RA. Lastly, bracing will help stabilize the foot joints, limit deformities and decrease pain.
In severe cases, surgery may be a treatment option that should be considered. For those who cannot walk without experiencing pain and those whose deformities can not be managed with braces, surgery should be considered. Your podiatrist will recommend surgery if he or she believes it will improve your foot biomechanics.
 Research has shown that many patients notice the first signs of the medical condition known as rheumatoid arthritis as appearing in the feet. Some of these symptoms may include swelling, instability, and pain that may originate from the changing foot bones. The part of the foot that is generally affected with this condition are the smaller joints of the toes, and occasionally, the ankle joint may experience symptoms. This ailment may typically cause severe pain and discomfort, and the toes will often look curled and deformed. This condition may be linked to additional foot ailments occurring, including nodules forming in the heel area and changes in the skin and nails. Additionally, it is noted that some patients may notice pain in the leg, which may be a result of a diminished blood supply. If you notice any signs that may indicate rheumatoid arthritis, it is suggested to speak to a podiatrist who can properly guide you to the best treatment options.
Research has shown that many patients notice the first signs of the medical condition known as rheumatoid arthritis as appearing in the feet. Some of these symptoms may include swelling, instability, and pain that may originate from the changing foot bones. The part of the foot that is generally affected with this condition are the smaller joints of the toes, and occasionally, the ankle joint may experience symptoms. This ailment may typically cause severe pain and discomfort, and the toes will often look curled and deformed. This condition may be linked to additional foot ailments occurring, including nodules forming in the heel area and changes in the skin and nails. Additionally, it is noted that some patients may notice pain in the leg, which may be a result of a diminished blood supply. If you notice any signs that may indicate rheumatoid arthritis, it is suggested to speak to a podiatrist who can properly guide you to the best treatment options.
Because RA affects more than just your joints, including the joints in your feet and ankles, it is important to seek early diagnosis from your podiatrist if you feel like the pain in your feet might be caused by RA. For more information, contact Dr. Alan J. Spector of Shore Podiatry. Our doctor will assist you with all of your podiatric concerns.
What Is Rheumatoid Arthritis?
Rheumatoid Arthritis (RA) is an autoimmune disorder in which the body’s own immune system attacks the membranes surrounding the joints. Inflammation of the lining and eventually the destruction of the joint’s cartilage and bone occur, causing severe pain and immobility.
Rheumatoid Arthritis of the Feet
Although RA usually attacks multiple bones and joints throughout the entire body, almost 90 percent of cases result in pain in the foot or ankle area.
Symptoms
Diagnosis
Quick diagnosis of RA in the feet is important so that the podiatrist can treat the area effectively. Your doctor will ask you about your medical history, occupation, and lifestyle to determine the origin of the condition. Rheumatoid Factor tests help to determine if someone is affected by the disease.
If you have any questions please feel free to contact our office located in Point Pleasant, NJ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Read more about Rheumatoid Arthritis in the FeetTarsal tunnel syndrome is a condition in which the tibial nerve, located in the tarsal tunnel in the foot, is compressed. The tibial nerve can become compressed from injury, such as an ankle sprain, flat feet, and lesions. Arthritis, diabetes, and varicose veins can also cause swelling and thus result in nerve compression.
Symptoms of tarsal tunnel syndrome include several different sensations in the sole of the foot, inside the ankle, and around the tibial nerve. These sensations include shooting pains, numbness or reduced sensation, pins and needles, burning, and tingling. Symptoms tend to worsen with greater activity to the area. In rare and severe occasions, this can change the muscles in the foot.
If you suspect you have tarsal tunnel syndrome, you should consult with your podiatrist. He or she will examine your medical history to see if you have a history of diabetes, arthritis, or flat feet. They will also check to see if you have suffered an injury to the area recently. An electrical test will be conducted to check if the nerve has been damaged. A simpler Tinel’s Test might also be used. This includes simply tapping the nerve to create a sensation. An MRI scan of the area may also be used.
Treatments vary greatly for tarsal tunnel syndrome. Treatments include both nonsurgical and surgical options depending upon the severity of the condition. Nonsurgical options include anti-inflammatory medication and steroid injections to the area. Orthotics, such as a splint or brace that immobilizes the foot, is another noninvasive option. For those with flat feet, custom shoes can be made to offer better foot support. Surgical options include a tunnel tarsal release, in which an incision is made behind the ankle down to the arch of the foot. This releases the ligament and relieves pressure off the nerve. Some doctors use a more minimally invasive surgery, where smaller incisions are made in the ankle and the ligament is stretched out.
If you are suffering from painful sensations in your foot, see a podiatrist who can determine if you are experiencing tarsal tunnel syndrome. Tarsal tunnel syndrome that is left unchecked can cause permanent nerve damage to the foot.
 The area in the foot that is located between bones and fibrous tissue is known as the tarsal tunnel. There are several nerves, arteries, veins, and tendons that lie inside this portion of the foot. If these nerves should be compressed, inflammation may occur and may be indicative of a condition that is referred to as tarsal tunnel syndrome. This uncomfortable ailment may be the result of different forms of arthritis, tumors that may be benign, or from a possible fracture. Additionally, medical conditions including flat feet or specific foot deformities can cause narrowing of this “tunnel” and may precede the onset of this condition. Patients will typically be aware of noticeable symptoms that may include numbness or tingling over the sole of the foot, in addition to pain and a burning sensation. If you feel you may have tarsal tunnel syndrome, it is advised to consult with a podiatrist who can perform a proper diagnosis and discuss correct treatment options.
The area in the foot that is located between bones and fibrous tissue is known as the tarsal tunnel. There are several nerves, arteries, veins, and tendons that lie inside this portion of the foot. If these nerves should be compressed, inflammation may occur and may be indicative of a condition that is referred to as tarsal tunnel syndrome. This uncomfortable ailment may be the result of different forms of arthritis, tumors that may be benign, or from a possible fracture. Additionally, medical conditions including flat feet or specific foot deformities can cause narrowing of this “tunnel” and may precede the onset of this condition. Patients will typically be aware of noticeable symptoms that may include numbness or tingling over the sole of the foot, in addition to pain and a burning sensation. If you feel you may have tarsal tunnel syndrome, it is advised to consult with a podiatrist who can perform a proper diagnosis and discuss correct treatment options.
Tarsal tunnel syndrome can be very uncomfortable to live with. If you are experiencing tarsal tunnel syndrome, contact Dr. Alan J. Spector of Shore Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome, which can also be called tibial nerve dysfunction, is an uncommon condition of misfiring peripheral nerves in the foot. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome, the tibial nerve is damaged, causing problems with movement and feeling in the foot of the affected leg.
Common Cause of Tarsal Tunnel Syndrome
The Effects of Tarsal Tunnel Syndrome
A physical exam of the leg can help identify the presence of tarsal tunnel syndrome. Medical tests, such as a nerve biopsy, are also used to diagnose the condition. Patients may receive physical therapy and prescriptive medication. In extreme cases, some may require surgery.
If you have any questions please feel free to contact our office located in Point Pleasant, NJ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Read more about Treating Tarsal Tunnel Syndrome